Two suspected cases of monkeypox in three local government areas of Anambra State have been recorded, as the victims are placed under surveillance.
TheNewsGuru.com (TNG) reports that the councils are Anambra East, Onitsha and Oyi.
Commissioner for Health Dr. Afam Obidike, who addressed reporters in Awka, said one of the cases has been confirmed positive. He added that the state emergency preparedness and response team put relevant surveillance measures in place towards curtailing the spread of the disease.
Obidike, however, urged residents not to panic but report to the hospital for proper examination whenever they notice rashes on their skin.
He said: “Few weeks ago, two suspected cases of monkey pox were reported in Anambra East, Onitsha and Oyi Local Government Areas. The case from Anambra East was confirmed positive and is currently receiving treatment at the isolation centre of the Nnamdi Azikiwe University Teaching Hospital in Nnewi.
“In light of the above, Governor Charles Soludo has declared the incident an outbreak, and an emergency preparedness and response committee meeting was convened on Wednesday. The meeting was attended by relevant stakeholders, including World Health Organisation (WHO) team and the United Nations International Children’s Emergency Fund (UNICEF); they are providing necessary assistance to the state.
“Planning for immediate response to the outbreak and surveillance, laboratory, case management, risk communication and community engagement, infection prevention and control and safe burial pillars were also activated.”
Obidike also announced the training of health personnel and response officers on enhanced active case search, sample collection and monkey pox management, as well as intensified public awareness.
The UK now has seven cases of monkeypox, an infectious disease that doesn’t spread easily between people. The first case on 7 May 2022 is thought to have been brought into the UK by a traveller returning from Nigeria.
Five things you need to know about Monkeypox
1. It’s caused by a smallpox-like virus
Monkeypox is caused by a virus of the same name that is closely related to smallpox, which has now been eradicated from the planet. Both are members of the Orthopoxvirus genus in the family Poxviridae. Monkeypox was first discovered in 1958 when outbreaks of a disease causing a pox were discovered in monkeys held in captivity for research. It was first seen in humans in 1970 in the Democratic Republic of the Congo (DRC) and it is now endemic in Central and West Africa.
In 2020, the World Health Organization (WHO) reported 4,594 suspected cases of monkeypox, including 171 deaths (case fatality ratio 3.7%). They are described as suspected because confirmation requires PCR testing, which is not easily available in endemic areas.
2. It causes pustules all over the body
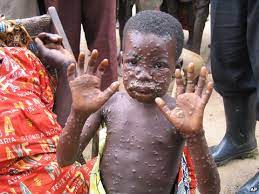
Symptoms normally appear between five and 13 days after infection, although it can take up to 21 days for them to appear. Early symptoms include fever, headache, muscle ache, backache, swollen lymph nodes, chills and exhaustion. Once fever has appeared, a rash tends to erupt, concentrated on the face, hands and feet before spreading to other areas of the body. It can spread to the inside of the mouth, the genitals and the cornea. The rash progresses until it forms a scab which falls off, and in some cases large sections of skin can drop off the body.
Although symptoms often ease within a month, one in ten cases can be fatal. Children are particularly susceptible.
3. Diagnosis requires PCR tests
Given that rashes are seen in many other diseases such as chickenpox and measles, WHO recommends diagnosis when identification is necessary. This has to be with PCR testing, they say, because orthopoxviruses produce antigens and trigger antibodies that could look like other related viruses, thus analyses of these cannot pinpoint that the virus is monkeypox.
4. It can spread between people through close contact
The virus generally spreads to people from infected wild animals such as rodents and primates, found in the rainforests of Central and West Africa, but human-to-human transmission can also occur. Similar to viruses like Ebola, transmission only happens in close proximity by contact with lesions, body fluids, respiratory droplets or contaminated materials such as bedding or clothes.
5. There’s currently no cure, but we have a (very old) vaccine
At present, there is no specific treatment recommended for monkeypox by WHO, but there are antivirals licensed to combat orthopoxviruses, such as tecovirimat.
The smallpox vaccine was key to eradicating smallpox decades ago, and this vaccine can be highly effective – 85% – in preventing monkeypox. However, the original first-generation smallpox vaccines are no longer available to the general public. A newer vaccinia-based vaccine was approved for the prevention of smallpox and monkeypox in 2019 but it is also not yet widely available.






